This post is from our archives and not all features will display correctly.
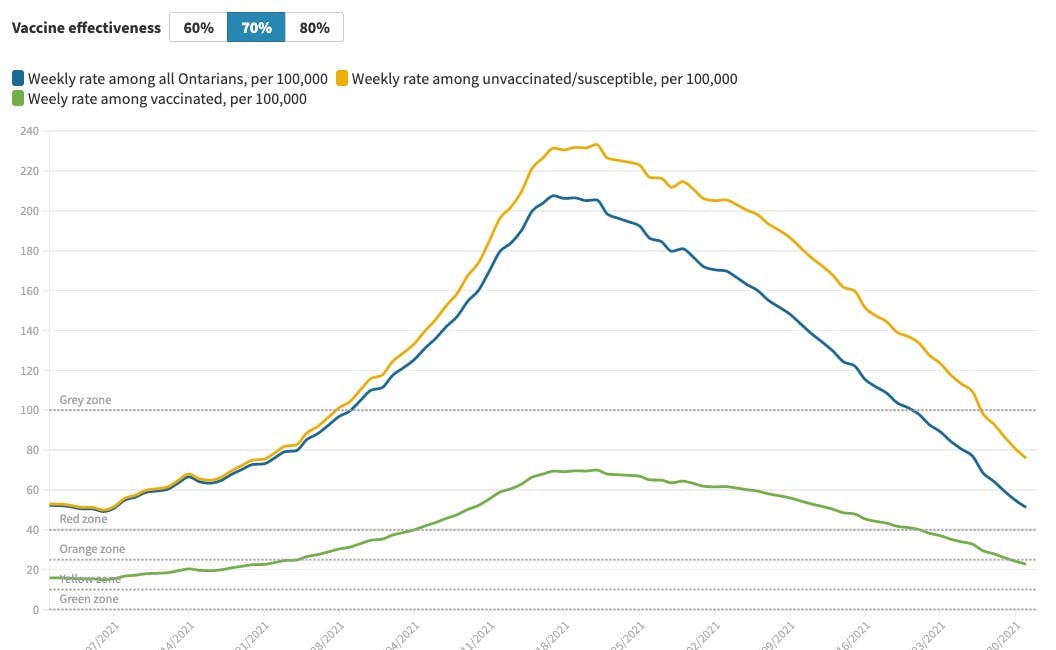
Data interactive: The unseen pandemic among susceptible Ontarians
As Ontario moves to lift restrictions, the unseen risk to unvaccinated people may rise considerably: epidemiologist.
Published May 31, 2021 at 4:33pm
Read this for free.
Log in below to get access to this article. One free per week.
