This post is from our archives and not all features will display correctly.
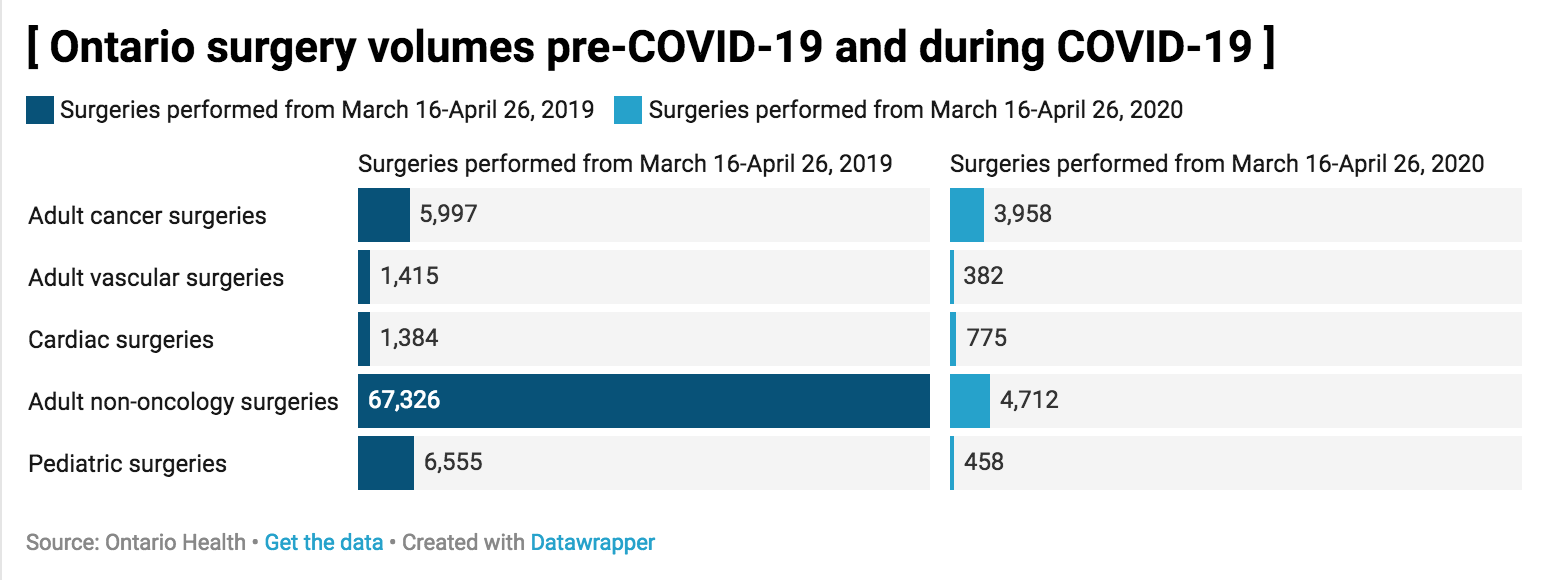
72,000 fewer surgeries performed in Ontario over six weeks of the COVID-19 pandemic
There were also 134,351 fewer CT scans and MRIs. Doctors say they aren’t surprised, but they are worried about the increased backlog.
Published May 11, 2020 at 5:16pm
Read this for free.
Log in below to get access to this article. One free per week.
