This post is from our archives and not all features will display correctly.
Ford calls for national contact tracing plan to contain COVID-19
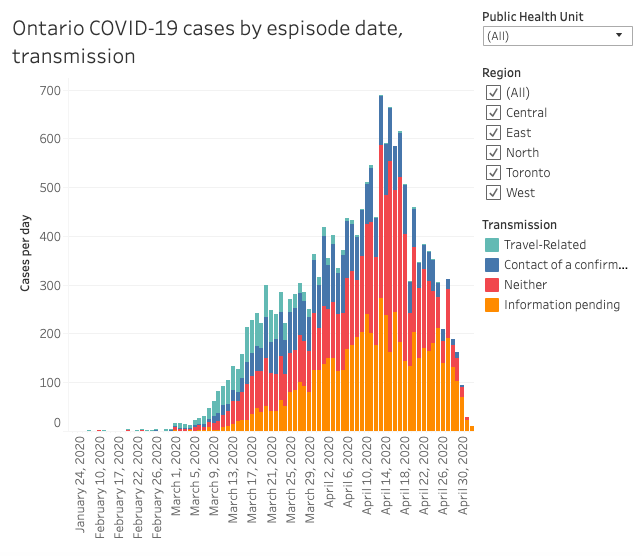
Ontario’s public health units were overwhelmed in March and could not keep up with the contact tracing and case management workload.
Published May 4, 2020 at 5:19pm
Read this for free.
Log in below to get access to this article. One free per week.
